The physiologist Hans Seyle (1907–1982) studied stress by examining how rats responded to being exposed to stressors such as extreme c old, infection, shock, or excessive exercise (Seyle, 1936, 1974, 1982). 1 Seyle found that regardless of the source of the stress, the ra ts experienced the same series of physiological changes as they suffered the prolonged stress. Seyle created the termgeneral adaptation syndrome to refer to thethreedistinct phases of physiological change that occur in responseto long-term stress:alarm,resistance, and exhaustion (Figure 10.5).

The experience of stress creates both an increase in general arousal in the sympathetic division of the autonomic nervous system (ANS), as well as another, even more complex, system of physiological changes through the HPA axis ((Reference None not found in Book)).
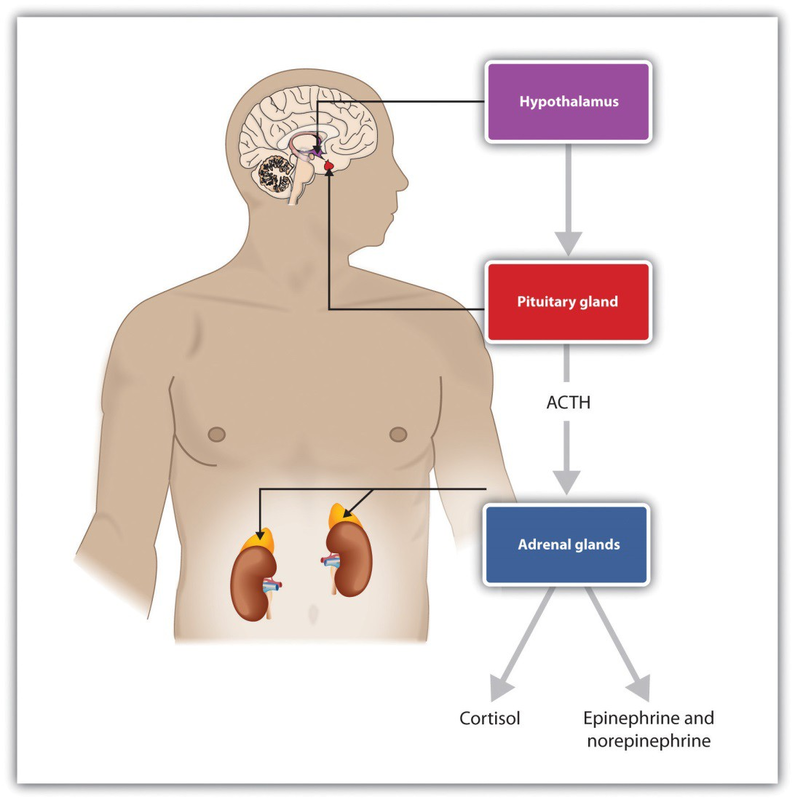
The HPA axis is a physiological responseto stress involving interactions among the hypothalamus, thepituitary, and theadrenal glands. The HPA response begins when the hypothalamus secretes releasing hormones that direct the pituitary gland to release the hormone ACTH. ACTH then directs the adrenal glands to secrete more hormones, including epinephrine, norepinephrine, and cortisol, a stress hormonethat releases sugars into theblood, helpingpreparing thebodyto respond to threat (Rodrigues, LeDoux, & Sapolsky, 2009). 2
The initial arousal that accompanies stress is normally quite adaptive because it helps us respond to potentially dangerous events. The experience of prolonged stress, however, has a direct negative influence on our physical health, because at the same time that stress increases activity in the sympathetic division of the ANS, it also suppresses activity in the parasympathetic
division of the ANS. When stress is long-term, the HPA axis remains active and the adrenals continue to produce cortisol. This increased cortisol production exhausts the stress mechanism, leading to fatigue a nd depression.
The HPA reactions to persistent stress lead to a weakening of the immune system, making us more susceptible to a variety of health problems including colds and other diseases (Cohen & Herbert, 1996; Faulkner & Smith, 2009; Miller, Chen, & Cole, 2009; Uchino, Smith, Holt- Lunstad, Campo, & Reblin, 2007). 3 Stress also damages our DNA, making us less likely to be able to repair wounds and respond to the genetic mutations that cause disease (Epel et al., 2006). 4 As a result, wounds heal more slowly when we are under stress, and we are more likely to get cancer (Kiecolt-Glaser, McGuire, Robles, & Glaser, 2002; Wells, 2006). 5
Chronic stress is also a major contributor to heart disease. Although heart disease is caused in part by genetic factors, as well as high blood pressure, high cholesterol, and cigarette smoking, it is also caused by stress (Krantz & McCeney, 2002). 6 Long-term stress creates two opposite effects on the coronary system. Stress increases cardiac output (i.e., the heart pumps more blood) at the same time that it reduces the ability of the blood vessels to conduct blood through the arteries, as the increase in levels of cortisol leads to a buildup of plaque on artery walls (Dekker et al., 2008). 7 The combination of increased blood flow and arterial constriction leads to increased blood pressure (hypertension), which can damage the heart muscle, leading to heart attack and death.
- 2745 reads






